In This Issue:
- Healthcare Industry Goes Toe to Toe with Physician Shortage, a Too-Familiar Foe
- AdventHealth’s Chief Clinical Officer Shares Efforts to Address Shortages
- Cross Country: Using a Locums Agency to Reduce Staffing Shortages in 2023
- SIA Report Addendum: Allied Resources Graduates to “Largest Staffing Firm”
- MPLT: 3 Critical Reasons Healthcare Facilities are Using Locums to Overcome Shortages
- Montana Hospitals Struggle as Anesthesiologist Shortages Persist
- Health Carousel Staffing Solution: Optimizing Patient Throughput
- Cross Country Healthcare Names Eric Christianson senior VP for Business Intelligence
- Medicus Promotes Heather Croke to Chief People Officer
- What to Do in San Antonio near the 2023 NAPR/NALTO Conference
- Join AAPPR in Austin for the 2023 AAPPR Annual Conference
- Socially Speaking: Social Posts of Note from All-Star, Georgia Medical, Hayes, LocumTenens.com, Wilderness, Weatherby, VISTA, MPLT, Cross Country & more
- How ‘Bout This: Longer Working Hours for Physician Mothers, Impact of Telemedicine on Ryan Haight Act, AMA’s New Plan
Got news? Submit it here, and we’ll include it in a future Locums Digest.
Healthcare Industry Goes Toe to Toe with Staff Shortages, a Too-Familiar Foe
(Edited from Medical Economics, 12/29/2022)
In a Medical Economics physician survey, staffing emerged as a top issue for physicians heading into 2023. This situation will likely worsen as an MGMA survey reveals that inadequate staffing is a growing concern for physicians. Most physicians across various roles reported 73% of practices experienced significant or moderate shortages, according to The Physicians Foundation.
“What we’re seeing across the board, regardless of whether it’s a physician-owned or hospital-owned practice, is that it’s a challenge to recruit and retain support staff,” says Ron Holder, MHA, chief operating officer for MGMA. “And support staff — medical assistants, nurses, and office staff — are critically important for physicians’ practices to succeed. And their challenges are compensation and costs keeping with inflation.”What are the best ways to keep clinicians and find new ones?
All the strategies recommended for 2022 — increasing pay and perks, having flexible work hours, listening to clinicians’ suggestions for workplace improvement, and more — will remain top solutions in 2023. The following tips will help enhance your recruitment and retention this year.
Get ready to pay, especially for office staff. Holder notes businesses, such as restaurants, retailers, or other businesses, may have to be prepared to pay more, especially for office staff. He notes when these businesses pay more than doctors’ practices, clerical workers can take their organization; and customer service skills where they can make more money.
All staff should work at the top of their license. Holder suggests all staff should do what they were trained to do and not have to do things that other people in the practice could effectively do at a lower level of licensure. It is important to maximize licensure at every level.
Find ways to manage the workload. The practice is shorthanded, don’t just pile more work onto everyone else. That can lead to feelings of dissatisfaction and make employees look for new jobs as Holder says. Then, if they leave that could worsen the situation. Some MGMA members reported closing practices one additional day a week to spread staff across their locations to avoid cutting hours.
For smaller practices, embrace flexibility. Staff crunches in large health systems lead to analyses about pay changes for dozens, perhaps hundreds, of employees. However, small practices don’t have that burden. Holder notes a practice with only two medical assistants and one leaves, then adjusting the practice’s pay grade on the fly to recruit back for that one.
Be equitable and fair when it comes to pay. Although early careerists with one to two years of experience are sparking bidding wars in the hunt for new workers, Holder says they should not start at higher salaries than staff with more experience.
Move new staff quickly to the midpoint. Recruiting and retaining staff with minimum qualifications and less experience often are more difficult than keeping those with 10 or more years of experience and who may stay with an organization for reasons beyond just a salary.
Streamline, streamline, streamline. Look for ways that every worker can reduce the number of clicks to complete tasks and for ways that medical assistants can help with a record entry and patient intake.
AdventHealth’s Chief Clinical Officer Shares Efforts to Address Shortages
(Lightly edited from Health Leaders Media by Christopher Cheney, 12/28/2022)
The shift of medical services from the hospital setting to the ambulatory setting and the home will accelerate in 2023, the chief clinical officer of AdventHealth’s Central Florida Division predicts.
HealthLeaders recently talked with Finkler about a range of issues, including clinical care predictions for 2023, the challenges he faces as a chief clinical officer, physician burnout, and workforce shortages. The transcript of that conversation below has been edited for brevity and clarity.

Neil Finkler, MD, chief clinical officer of AdventHealth’s Central Florida Division. Photo courtesy of AdventHealth.
HL: What kind of workforce shortages are you experiencing at AdventHealth?
Finkler: We have workforce shortages not only in the nursing area but also in other disciplines, including pharmacy, radiology, laboratory technicians, and certified registered nurse anesthetists. It is important for everybody to recognize that the shortages do not stop in the nonphysician side—we are seeing physician shortages in several specialties.
HL: What are the primary efforts you have in place to address workforce shortages?
Finkler: The first thing we have done as an organization is taken a step back and said, ‘We understand that pay must be competitive.’ In the pre-pandemic era, we would do market surveys every year or every other year. Now, we need to conduct market surveys more frequently. What was competitive a week ago may not be competitive four weeks from now. We are making sure that we are paying at the top of the market.
However, it is not just pay that is contributing to workforce shortages. It is also about benefits. I am proud of our nursing innovation and workforce strategies that have helped stem the tide. We have gone from 3% turnover per month down to 1% per month. Things like working in a team model have helped.
We also are working on virtual nursing models. We recognize that we have a paucity of experienced nurses. Many of our nurses are young—many are graduate nurses. They do not have an enormous amount of experience, and they do not have a seasoned nurse to turn to on the floor. So, we have been working with experienced nurses in a virtual nurse model where they can cover several units in a hospital. They help the nurses on the floor with problems and questions, and they can do work such as discharges.
We have told our nurses if they want to go back to school to continue their education, we will pay for it, and they will be debt free. We also have been providing nurses with more flexibility in scheduling. So, we are taking a proactive approach to the nursing shortage.
All News Is Locums
Cross Country: Using a Locums Agency to Reduce Staffing Shortages in 2023
(Lightly edited from Cross Country Locums, 12/6/2022)
In a December blog post, Cross Country explored how locums agencies can reduce staffing shortages in 2023. Among other things, locum tenens can alleviate pressures on permanent providers, expand telehealth offerings, and fill hard-to-fill specialties to improve patient wait times.
Healthcare leaders should keep these pressing workforce issues in mind this year.
Getting Ahead of Workforce Deficits
The healthcare industry faces pressing issues such as understaffing, provider wellness, and patient loyalty. A significant issue is the healthcare staffing deficit. The number of nurses in the US dropped 12.5% from 2021 to 2022, and 58% of medical practices reported staffing as their biggest challenge.
The nurse shortage may reach over 500,000 by 2030. To address this, healthcare organizations can attract and retain providers by providing competitive pay, career growth, autonomy, flexibility, and effective leadership. They can also access a pool of high-quality candidates through in-house or outsourced staffing resources and implement a strategy for ongoing locum tenens support to adjust staff as needed.
Supporting Provider Wellness
Another crucial concern is the well-being of healthcare providers. A majority of physicians, 62.8%, are experiencing burnout, and 52.59% are reporting episodes of depression, according to a Mayo Clinic report. To address this, healthcare organizations should implement strategies to support their providers’ mental health and well-being. Healthcare organizations can support providers’ well-being by using locums, providing resources for stress management, showing appreciation, and fostering diversity.
Building Patient Loyalty
Healthcare organizations also need to focus on building patient loyalty. With the increasing popularity of telehealth and the entry of retail companies into the healthcare industry, traditional healthcare providers may need help retaining patients. According to Deloitte, 80% of consumers surveyed reported they are likely to have another virtual visit, even post-COVID-19. To attract and retain patients, healthcare organizations should offer easy access, fast digital communication, short wait times, positive provider interactions, and an inclusive environment. Organizations implementing these strategies can thrive in a “patient experience economy” and build loyalty among healthcare consumers.
SIA Report Addendum: Allied Resources Medical Staffing Graduates to “Largest Staffing Firm”
(Lightly edited from Staffing Industry Analysts, 12/13/2022)
In August, Staffing Industry Analysts published its annual rankings of the “Largest Healthcare Staffing Firms in the US.” SIA’s 2022 report was updated in December with new information about companies that could’ve been included in the initial report.
One of those companies was Allied Resources Medical Staffing. The report details that Allied generated $110 million in U.S. staffing revenue in 2021, the vast majority of which — $106 million — was generated from nurse staffing.
In our Locums Brief published in September that covered the SIA report, Aya Healthcare topped the list of the biggest healthcare staffing companies and came home with the #2 spot on SIA’s “Largest US Staffing Firms.” Of the 81 healthcare staffing agencies included in the report, 26 were new to the list.
Rounding out the list with six rising companies making the rankings for the first time were Atrium Health, DRW & MSI Group, Floyd Lee Locums, Ingenovis Health, Loyal Source, and OR Nurses Nationwide — a nurse staffing firm that claims to staff locums as well.
SIA members can access the full report here.
MPLT: 3 Critical Reasons Healthcare Facilities are Using Locums to Overcome Shortages
(Lightly edited from MPLT Healthcare, 12/27/2022)
The demand for healthcare employees in all areas of medicine continues to rise as healthcare facilities and hospitals increasingly rely on locum tenens providers to fill staffing gaps.
Over the last several years, locum tenens clinicians have provided significant support to existing medical teams, assisting with patient care on all levels. These are the three reasons why more healthcare facilities are using locum tenens providers for coverage:
1. Alleviates provider burnout
Locum tenens providers help alleviate burnout among full-time healthcare staff by filling in during peak times and assisting overburdened units such as ER during holidays when permanent staff are off, thus relieving the pressure on full-time staff.
2. Accelerates the hiring process
Locum tenens providers accelerate the hiring process by allowing healthcare facilities to quickly fulfill staffing needs without going through the lengthy process of vetting, interviewing, training, and onboarding permanent staff. They are connected to healthcare organizations through staffing agencies and have already been vetted through an extensive medical credentialing process, allowing facilities to quickly hire reliable providers when needed.
3. Telemedicine allows more patient access
Telemedicine allows for more patient access and as it becomes more mainstream, facilities need experienced healthcare providers to help deliver telehealth services effectively. Locum tenens providers with experience in telecommunications technology are in high demand during peak patient volume times, such as winter. As telemedicine continues to grow, locum tenens providers will play an important role in serving patients through virtual platforms. The demand for locum providers is expected to increase, and facilities that use them will have support to overcome staffing challenges even during busy times.
Montana Hospitals Struggle as Anesthesiologist Shortages Persist
(Lightly edited from Billings Gazette by Emily Schabacker, 1/6/2023)
Billings Gazette recently wrote about how hospitals across the country are struggling to find solutions as anesthesiologist shortages persist. The shortage is especially acute in rural states like Montana, where medical professionals have long been in short supply. To keep up, hospitals are increasingly relying on traveling anesthesiologists, known as “locum tenens.”
Additionally, many hospitals use Certified Registered Nurse Anesthetists (CRNA) to fill the gap. However, some physician anesthesiologists argue that CRNAs lack the skill set and training to care for sick patients at regional hospitals. This issue has reached a critical point due to increasing burnout among providers and their growing desire for better work-life balance.
Read the full story to learn how one rural clinic addressed its staff shortage.
Health Carousel Staffing Solution: Optimizing Patient Throughput
(Lightly edited from Health Carousel Locum Tenens, 1/9/2023)
In a recent blog post, Health Carousel explored how hospitals can solve staffing shortages by optimizing patient throughput. Hospitals can implement this strategy to boost efficiency, increase patient access to care, and see a positive impact on their bottom line.
The key to achieving this is ideal bed management, which involves shortening patient stay, streamlining communication and teamwork, and using locum tenens providers. Hospitals can improve patient throughput and quality of care by identifying areas of need and using locums. Locums, in turn, can boost bed turnaround time, increase overall efficiency, and ensure that urgent admissions have shorter wait times.
The ultimate benefits of improving patient throughput include better care, better hospital performance, increased efficiency, and financial returns. Hospitals can improve patient throughput and achieve organizational growth by evaluating needs and strengthing current systems.
Learn more about reducing staffing shortages by optimizing patient throughput in Health Carousel’s post.
The Healthcare Staffing Story
Cross Country Healthcare Names Eric Christianson Senior Vice President for Business Intelligence
(Lightly edited from Business Wire post, 1/9/2023)
Cross Country Healthcare, Inc. has announced that Eric Christianson joined the Company on January 9, 2023, to serve as its Senior Vice President, Intellify Solutions. Christianson will report to the Company’s Chief Commercial Officer, Dan White.
“I’m thrilled that Eric has joined Cross Country to accelerate the Company’s growth trajectory leveraging our new SaaS-based proprietary vendor-neutral platform, Intellify. Eric has been pioneering digital transformations and delivering innovative solutions through technology for nearly 20 years with a proven track record of high-growth business outcomes and significant client impact,” said White.
Before joining the Company, Christianson served as President, Digital Transformation at Triage Staffing since February 2022. Most notably, he co-founded Medefis, which AMN Healthcare acquired in January 2015. Christianson served as the Chief Operating Officer of Medefis from 2003 through January 2022 and as its President from January 2014 through January 2022.
“Eric brings a tremendous amount of expertise and leadership as we continue to develop and deploy innovative integrated solutions designed to address our clients’ most challenging workforce needs for both permanent and contingent labor,” said John A. Martins, CEO and President of Cross Country Healthcare. “Eric is well respected in the industry and will fuel the expansion of our technology strategy delivering greater efficiencies, transparency, and cost containment in the marketplace to more effectively manage clinical labor,” he continued.
Medicus Healthcare Solutions Promotes Heather Croke to CPO
(Lightly edited from PRWeb by Jessica Alberico, 1/10/2023)
Medicus Healthcare Solutions announced the promotion of Heather Croke to Chief People Officer. In this new role, Heather, who has led the People Team since 2021, will continue to drive the company’s core people strategy and operations as a member of the C-Suite.

As Chief People Officer, Heather will provide strategic direction for human resources, learning and development, talent acquisition, internal communications, and employee engagement.
In her current role as Vice President of People, Risk, and Strategy, Heather has played a critical role in advancing Medicus’ “People First, Always” approach, ensuring that Medicus is a top employer in New Hampshire and is a workplace where employees can thrive.
“A company like Medicus doesn’t succeed without its most valuable resource – people. Our people are our differentiators. Under Heather’s direction, we have built – and will continue to develop – a culture that is vital to our company’s success,” said Bob Dickey, Chief Executive Officer. “As a trusted advisor and an integral member of our leadership team, Heather has aligned our people strategy with the company’s strategic initiatives and will continue to do so in this new role.”
Recently, under Heather’s leadership, Medicus earned the DecisionWise Employee Engagement Top Performer Award. This award spotlights organizations that have finished in the top 10% for overall employee engagement scores in 3 company size tiers: less than 1,000 employees, 1,000-4,999 employees, and 5,000+ employees.
Tools to Try/News to Use
What to Do in San Antonio near the 2023 NAPR/NALTO Conference Site
(Edited from NALTO web page, 1/10/2023)
Heading to the upcoming NALTO conference from February 5 to 7? Here are some must-see sights and activities to check out while in San Antonio.
Start by taking a stroll along the iconic River Walk. This picturesque area is lined with shops and restaurants, offering the perfect spot to grab a souvenir or enjoy a meal al fresco. Take the barge to explore all the River Walk has to offer.
Next, head to the world-famous Alamo, just a short walk away. Here you can tour the historic buildings and gardens and view artifacts from its storied past. While at the Alamo, take advantage of the opportunity to visit the San Antonio Missions National Park, which connects four Spanish Missions along eight miles of walking and biking trails.
For those interested in historical architecture, take a quick walk to check out the King William Historic District. This 25-block area south of downtown features Victorian, Greek Revival, and Italianate-style grand homes. The San Antonio Conservation Society provides self-guided tour information for this area.
Don’t Miss The Opening Keynote Speaker

This session will empower leaders to unlock the secrets to leading and managing a team of leaders with this powerful opening keynote speaker. This session is a must-attend for anyone looking to empower their team and drive success, teamwork, and profitable growth.
Learn key strategies for effective communication, team development, creating a positive work environment, coaching to performance standards, conflict resolution, and team building through interactive exercises and discussions. By the end of the session, participants will have the confidence and tools needed to lead and manage a team of leaders to drive success, teamwork, and profitable growth.
NALTO® Membership Applications Now Open
Don’t miss out on the opportunity to be a part of a community of industry leaders!
In becoming a NALTO member, you will gain access to exclusive resources and opportunities to network with top industry professionals.
Learn more about and apply for a NALTO membership here.
Join AAPPR in Austin for the 2023 AAPPR Annual Conference!

Join 1,000 professionals at this year’s Association of Advancing Physician and Provider Recruitment (AAPRR) Annual Conference on March 21-24 at the Austin Convention Center.
The event offers opportunities to learn from experts, network, acquire knowledge about industry trends, and have fun.
You can have a booth or sponsor the event, or advertise in the onsite program. You can also register to be a speaker.
Visit the AAPPR conference site for more information and registration details.
How ‘Bout This?
20 Years of Longer Working Hours for Physician Mothers
(Lightly edited from Healio by Andrew Rhodes, 1/2/2023)
A new study in JAMA Internal Medicine has found that while physicians’ average number of hours worked has decreased since 2001, physician mothers have seen an increase in their weekly work hours. The study’s lead author, Dr. Anna Goldman, suggests this could signify progress in career engagement for women in medicine. Dr. Goldman also highlights that it could contribute to high burnout rates among physician mothers reported in previous studies.
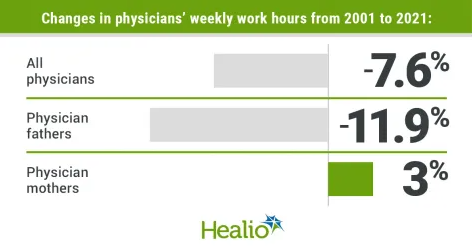
The study analyzed federal survey data from 2001 to 2021 on the weekly work hours of 36,137 physicians, 12,120 of which were women. The data showed that the physician workforce grew by 32.9% overall but fell by 6.7% during the pandemic.
Weekly work hours for physicians dropped by 7.6%, from 52.6 hours in 2001 to 48.6 hours in 2021. Male physicians, physician fathers, and rural physicians drove most of the decrease.
Physician mothers’ bucked this trend. Their weekly hours increased by 3%, from 42.7 to 43.9, in contrast to physician fathers. The researchers suggest this could aid in addressing the gender pay gap in medicine, but only in terms of total hours worked and not revenue generated per hour. Longer working hours for physician mothers may indicate improved accommodation in the workplace but does not necessarily equate to progress in achieving gender equity in balancing household and work responsibilities.
Read more to see how mothers in the advanced practice professional workforce have been impacted by this trend.
The Impact of Telemedicine on Ryan Haight Act
(Lightly edited from Psychology Today by Joel L Young, M.D., 1/11/2023)
The Ryan Haight Act of 2008 regulates the prescription of controlled substances and requires a doctor-patient relationship. The act requires clear guidelines for in-person evaluations and needs to update its exceptions to accommodate the uptick in telemedicine. As telemedicine becomes increasingly vital for patient care, revisions to the act may be necessary to protect healthcare providers and ensure patient access to care.
Read more about the act and its potential impact on telemedicine.
AMA Empowers Patients, Physicians in 2023 Plan
(Lightly edited from AMA by Andis Robeznieks, 1/6/2023)
Last year was a tough one for patients and physicians, but momentum is building to reform the broken Medicare physician payment system in 2023 and to reduce obstacles that interfere with patient care—including prior authorization. There are also now better tools to keep up the fight against COVID-19.
Despite progress, there are still unacceptably high rates of burnout among physicians, science and medicine remain under attack in social media and state capitols, and the nation is dealing with the “tripledemic” brought on by increases in seasonal influenza, respiratory syncytial virus infection (RSV), and COVID-19.
“The last few years have been a bit of a blur, but last year about this time, we were blindsided with Omicron,” along with major increases in hospitalizations, said AMA President Jack Resneck Jr., MD. However, he added, “I do think we’re in a better place,” Dr. Resneck said, adding that people who have not received their COVID-19 bivalent booster vaccination should do so.
Dr. Resneck spoke during a recent episode of “AMA Update,” in which he explained how 2023’s challenges could be met through the AMA Recovery Plan for America’s Physicians. The plan aims to fix prior authorization, improve medicare pay, stop scope creep, promote telehealth, and reduce physician burnout.
Watch the latest episode on what AMA’s top concern is this year.